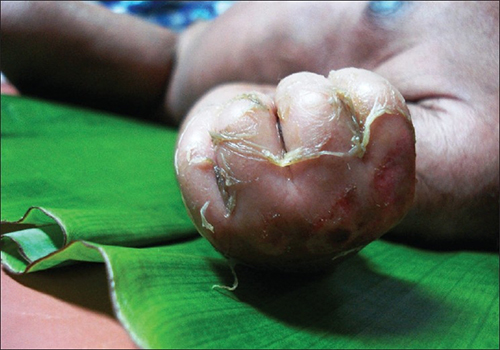
Staphylococcal Scalded Skin Syndrome: Unraveling the Condition
Imagine a child's skin, once soft and smooth, suddenly appearing as if it's been scalded by hot liquid, peeling away in large sheets. This alarming presentation is the hallmark of Staphylococcal Scalded Skin Syndrome (SSSS), a rare but severe superficial blistering skin disorder. Far from a simple rash, SSSS is a critical medical emergency that demands immediate attention. It's often referred to interchangeably with the eponymous Ritter von Ritterschein disease, or simply Ritter disease, particularly when it affects the most vulnerable — newborn children.
At its core, Staphylococcal Scalded Skin Syndrome is not a burn, despite its appearance. Instead, it's a profound reaction triggered by the release of powerful exotoxins from specific strains of Staphylococcus aureus bacteria. While *Staphylococcus aureus* is a common bacterium that can reside harmlessly on the skin or in the nose of many individuals, certain strains produce toxins known as exfoliative toxins. These toxins target a specific protein (desmoglein 1) responsible for holding the outermost layer of skin cells (the epidermis) together. When this bond is broken, the superficial layer of the skin detaches, creating the characteristic blistering and peeling that mimics severe burns.
Understanding the bacterial origin and the mechanism of toxin action is crucial for both diagnosis and treatment. Unlike some skin infections where the bacteria directly invade the skin, in SSSS, it's the *distant effect* of the toxins circulating in the bloodstream that causes widespread skin damage, even if the initial infection site is small or hidden.
Who is at Risk? Identifying Vulnerable Populations and Triggers
While Staphylococcal Scalded Skin Syndrome can occur at any age, certain populations are disproportionately affected. Children, especially those younger than six years old, face the highest risk. Their immune systems are still developing, making them more susceptible to the systemic effects of the bacterial toxins. This vulnerability is a key reason why prompt recognition in pediatric cases is so vital. You can learn more about specific risks and underlying causes by reading our detailed article: Understanding SSSS in Children: Causes, Symptoms & Treatment.
Beyond age, several other factors can increase an individual's susceptibility to SSSS:
- Weakened Immune System: Individuals with compromised immune systems, due to illness, medication, or underlying conditions, may struggle to neutralize the bacterial toxins effectively, leading to more severe and widespread skin detachment.
- Chronic Kidney Disease or Kidney Failure: The kidneys play a crucial role in filtering toxins from the body. In patients with kidney dysfunction, the exfoliative toxins may not be cleared efficiently, allowing them to accumulate and cause more extensive skin damage. This highlights the importance of considering a patient's overall health status when evaluating for SSSS.
Interestingly, some studies suggest a seasonal prevalence, with SSSS appearing more frequently during the summer and fall months. While the exact reasons for this trend are not fully understood, it may be linked to environmental factors or common seasonal infections that could indirectly impact immune responses or *Staphylococcus aureus* prevalence.
Recognizing the Red Flags: Symptoms of SSSS
The symptoms of Staphylococcal Scalded Skin Syndrome can develop rapidly and can vary slightly from person to person, or child to child. Being vigilant for these warning signs is paramount for early diagnosis and intervention. The disease often begins subtly, making early detection a challenge, but progresses quickly to its more alarming manifestations.
Initial Symptoms (Often Preceding Widespread Skin Changes):
- Fussiness or Irritability: Especially in infants and young children, an unexplained increase in irritability can be an early indicator of discomfort or illness.
- Tiredness or Lethargy: A notable decrease in energy levels or unusual drowsiness can signal a systemic infection.
- Fever: This is a common response to infection and typically accompanies the onset of SSSS.
- Redness of the Skin: The skin may initially appear diffusely red, often starting around the mouth and nose, before spreading to other areas. This redness can sometimes be mistaken for sunburn or another widespread rash.
Progressive and Characteristic Symptoms:
- Fluid-Filled Blisters: Within hours or a day of the initial redness, fragile, fluid-filled blisters begin to form on the skin. These blisters are often shallow and break easily, exposing moist, raw, and incredibly tender skin underneath.
- Peeling Skin: This is the most striking and diagnostic symptom. Large sheets of the top layer of skin (epidermis) peel away, leaving behind raw, painful, and often shiny areas that strongly resemble a severe burn. This extensive peeling can occur over large parts of the body, including the face, trunk, and extremities. The appearance can be truly shocking to caregivers and medical professionals alike, underscoring the severity of the condition.
Given that SSSS symptoms can mimic other health conditions, such as severe allergic reactions or other blistering disorders, it is critical not to self-diagnose. If your child exhibits any combination of these symptoms, particularly red, blistering, or peeling skin, seek immediate medical attention. Swift action can make a profound difference in the outcome.
Diagnosis and Swift Action: How SSSS is Identified
Diagnosing Staphylococcal Scalded Skin Syndrome requires a keen clinical eye and often a rapid investigative approach. Due to its serious nature and the need for immediate treatment, healthcare providers prioritize a prompt and accurate diagnosis. The process typically begins with a thorough evaluation by a healthcare professional.
The Diagnostic Process:
- Medical History and Physical Exam: The provider will gather detailed information about the onset of symptoms, their progression, and any relevant medical history. A comprehensive physical exam will focus on the characteristic skin changes, including the extent of redness, blistering, and peeling. The "Nikolsky sign," where gentle pressure on seemingly unaffected skin causes the epidermis to shear off, is often present and highly indicative of SSSS.
- Skin Biopsy: A small tissue sample of the affected skin is taken and sent to a lab for microscopic examination. A crucial aspect here is the "frozen section" biopsy, which can be performed very quickly, providing a preliminary diagnosis within minutes to hours. This rapid confirmation is invaluable in initiating timely treatment. The biopsy helps distinguish SSSS from other conditions that cause blistering, such as autoimmune disorders.
- Cultures: To identify the specific bacterial culprit, cultures are taken from various sites. While the skin where the peeling occurs is often sterile (as it's the toxin, not the bacteria, causing the damage there), the source of the *Staphylococcus aureus* infection needs to be found. Common culture sites include:
- Blood
- Urine
- Nose and throat
- Areas of intact skin or potential infection (e.g., around the eyes, or the umbilical cord in newborns)
The speed of diagnosis is paramount. Every hour counts in preventing the disease from progressing further and mitigating potential complications. If a healthcare provider is unavailable, do not hesitate to go to the emergency room immediately if you suspect SSSS.
Comprehensive Care: Treating Staphylococcal Scalded Skin Syndrome
Treatment for Staphylococcal Scalded Skin Syndrome is multifaceted and typically aggressive, mirroring the care provided for severe burn patients. This comprehensive approach is essential to manage the extensive skin damage, prevent dehydration, and eradicate the underlying bacterial infection. The specific treatment plan will be tailored to the individual, considering their age, overall health, the severity of symptoms, and the extent of skin involvement. For a deeper dive into the recovery process, refer to our article: SSSS Explained: Diagnosis, Treatment, and Recovery Outlook.
Hospitalization and Specialized Care:
- Intensive Care Unit (ICU) or Burn Unit: Most patients with SSSS, especially children, will require admission to an ICU or a specialized burn unit. These units offer a sterile environment, continuous monitoring, and staff experienced in managing critical conditions, fluid balance, and severe skin injuries. The care is remarkably similar to that for thermal burns, focusing on protecting the raw skin surfaces and preventing secondary infections.
Key Treatment Modalities:
- Intravenous (IV) Antibiotics: This is the cornerstone of SSSS treatment. High-dose antibiotics, administered directly into a vein, are crucial to quickly eliminate the *Staphylococcus aureus* infection responsible for producing the exfoliative toxins. The specific antibiotic chosen will depend on the sensitivity of the bacterial strain identified in cultures.
- IV Fluids to Prevent Dehydration: The extensive skin peeling leads to a significant loss of body fluids, akin to what happens in a burn. IV fluids are essential to replace these losses, maintain hydration, and prevent dangerous electrolyte imbalances and shock.
- Pain Management: The exposed, raw skin is extremely painful. Potent pain medicines are administered to ensure the patient's comfort and allow for necessary wound care procedures.
- Skin Creams, Ointments, and Bandages: Gentle skin care is vital. Non-irritating creams and ointments are applied to the denuded areas to promote healing, prevent further damage, and reduce the risk of secondary infections. Sterile bandages are often used to protect the compromised skin and maintain a moist healing environment.
- Nasogastric (NG) Feeding: In severe cases, especially in infants or very ill children, oral feeding might be difficult or impossible due to pain, lethargy, or the risk of aspiration. Nasogastric tube feeding ensures adequate nutrition and caloric intake, which is crucial for healing and recovery.
Potential Complications and Prognosis:
With prompt and appropriate treatment, most children with SSSS recover fully without any scarring or long-term problems. The skin typically heals remarkably well once the toxin production is halted and the underlying infection is cleared. However, without timely intervention, serious complications can arise:
- Severe Dehydration and Shock: Extensive fluid loss can quickly lead to life-threatening dehydration and hypovolemic shock.
- Worsening Infection/Sepsis: The compromised skin barrier makes patients highly vulnerable to secondary bacterial infections, which can spread systemically and lead to sepsis.
- Scarring: While rare with proper care, deep skin damage or secondary infections could potentially lead to scarring.
- Death: Although uncommon with modern medical care, SSSS can be fatal, particularly in very young infants or individuals with severe underlying health issues if treatment is delayed.
The good news is that with vigilant care and modern medical interventions, the outlook for patients with SSSS is generally excellent. The key takeaway remains the critical importance of early recognition and immediate presentation to a healthcare provider.
Conclusion
Staphylococcal Scalded Skin Syndrome is a serious dermatological emergency characterized by skin peeling that tragically mimics severe burns. Caused by toxins released from specific strains of *Staphylococcus aureus*, it predominantly affects young children and individuals with compromised immune systems or kidney disease. Recognizing the tell-tale symptoms—from initial fussiness and fever to widespread blistering and peeling skin—is the first, crucial step toward a positive outcome. Rapid diagnosis, often involving skin biopsies and bacterial cultures, paves the way for aggressive treatment. With comprehensive care in specialized units, including IV antibiotics, fluid management, pain control, and meticulous skin care, most patients make a full recovery without lasting scars. Always remember: if you suspect SSSS, especially in a child, seek immediate medical attention. Swift action saves lives and ensures the best possible healing.